
Hyderabad: A blood test that doctors across India use every day to diagnose diabetes, and that insurance companies demand before issuing policies, may be systematically misleading millions of people, according to a comprehensive analysis published in The Lancet Regional Health – Southeast Asia.
What is the ‘misleading’ blood test?
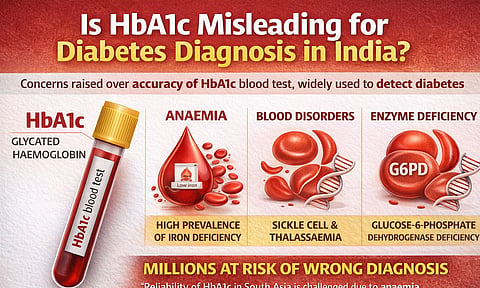
The test in question is HbA1c, or glycated haemoglobin, which has become the go-to method for detecting diabetes because it doesn’t require fasting and provides a snapshot of average blood sugar levels over two to three months.
But researchers warn that in India, where more than half the adult population suffers from anaemia and inherited blood disorders are common, the test can produce drastically inaccurate results, either missing diabetes cases entirely or falsely diagnosing healthy people.
“Glycated haemoglobin (HbA1c) is commonly used to diagnose and monitor type 2 diabetes (T2D). However, in South Asia, particularly India, the high prevalence of anaemia, hemoglobinopathies and glucose-6-phosphate dehydrogenase (G6PD) deficiency, and poorly standardised HbA1c assay methods complicates the interpretation of HbA1c values, challenging its reliability in both diagnosis and monitoring of diabetes,” the authors stated in their paper.
The implications extend far beyond individual patients.
India is home to more than 10 crore people with diabetes and crores more with prediabetes. If the primary test used to identify these conditions is unreliable for large sections of the population, it could mean the country’s entire understanding of its diabetes burden, and the policies built upon it, rests on shaky ground.
The iron deficiency problem
At the heart of the issue is a biological quirk: HbA1c measures diabetes by detecting glucose attached to haemoglobin in red blood cells. But anything that affects haemoglobin levels or the lifespan of red blood cells will distort the reading, regardless of actual blood sugar.
In India, that’s a massive problem.
According to the National Family Health Survey-5 conducted between 2019 and 2021, 57 per cent of women and approximately 25 per cent of men in the country are anaemic. A comprehensive meta-analysis cited in the paper found an overall anaemia prevalence of 53 per cent among adults aged 19–59 years, with regional variation ranging from 64 per cent in the Northern region to 39 per cent in the North-East. Among adults aged 60 years and older, prevalence ranged from 52 to 68 per cent.
Iron-deficiency anaemia, the most common form, alters how long red blood cells survive in the bloodstream. This can falsely raise or lower HbA1c values independent of actual blood sugar levels. The distortion is especially relevant in rural and underserved regions, where populations are nutritionally compromised and anaemia often goes undiagnosed or untreated.
But anaemia is just one piece of the puzzle. The paper highlights inherited blood disorders as equally problematic.
Sickle cell disease, sickle cell trait and various forms of thalassaemia affect millions of Indians, particularly in states like Madhya Pradesh, Chhattisgarh and Maharashtra, and especially among tribal populations. These conditions shorten red blood cell lifespan and alter haemoglobin structure, both of which compromise HbA1c reliability.
The silent enzyme deficiency is delaying diagnosis
Perhaps most alarming is the role of glucose-6-phosphate dehydrogenase (G6PD) deficiency, an X-linked enzymatic disorder that affects an estimated 8.5 per cent of the Indian population, with prevalence especially high in tribal groups.
The authors cite a major genomic study involving over 5,00,000 participants that identified substantial underdiagnosis of G6PD deficiency among South Asian males. The study found that carriers exhibited a mean HbA1c reduction of approximately 0.9 percentage points (approximately 10 mmol/mol) without a corresponding difference in mean blood glucose.
“Importantly, this discordance resulted in a median delay of 4.1 years in diabetes diagnosis and a 37 per cent increase in microvascular complications,” the authors noted, highlighting the real-world consequences of relying on HbA1c alone.
Even in the absence of overt symptoms, G6PD deficiency can silently shorten red cell lifespan, thereby lowering HbA1c values independently of actual blood sugar levels. This means people with diabetes may go years without knowing they have the condition, all the while developing complications like kidney damage, nerve problems and vision loss.
When two tests tell different stories
Multiple Indian studies reviewed by the authors show poor agreement between HbA1c and glucose-based tests such as the oral glucose tolerance test (OGTT).
In one South Indian study, OGTT detected nearly twice as many people with prediabetes as HbA1c. In another, HbA1c thresholds recommended by international guidelines missed up to two-thirds of prediabetes cases.
In young adults and anaemic populations, HbA1c frequently overestimates prediabetes prevalence, while in others, it failed to detect high post-meal glucose spikes that carry cardiovascular risk.
The authors point to a cross-sectional study of 1,120 Asian Indians in South India, where OGTT identified far more cases of prediabetes (87.8%) than HbA1c (45.4%), with minimal overlap.
In another study of 1,972 adults in north India, HbA1c cut-offs recommended by the American Diabetes Association and International Expert Committee showed moderate accuracy but significantly underdiagnosed prediabetes compared with the oral glucose tolerance test.
Laboratory chaos adds another layer
The problem isn’t just biological—it’s also technical. The authors flag inconsistent laboratory practices across India as a major concern. While HbA1c testing is widely available, many laboratories use non-standardised methods, and a significant proportion are not certified under international quality programmes.
A survey of 310 Indian laboratories found that 75 per cent used HbA1c for diabetes diagnosis, but only 70 per cent of these assays were National Glycohaemoglobin Standardisation Programme (NGSP)-certified. Participation in proficiency testing for HbA1c was limited, highlighting gaps in quality assurance.
Even commonly used techniques can give misleading results in people with silent haemoglobin variants. The authors cite a Spanish study of over 42,000 patients where 160 had abnormal chromatograms, and 134 showed significant discordance between HbA1c and fasting plasma glucose.
Adding to the confusion, seasonal fluctuations have been documented in Indian patients.
A study of 8,138 Indian patients found seasonal variations in HbA1c levels, with peaks during the monsoon (June–September) and the lowest levels in autumn (October–November), independent of long-term blood sugar control.
What should doctors do instead?
The researchers make clear recommendations for a better approach.
“Overall, reliance solely on HbA1c is constrained by several clinical and biological factors in India. A multiparametric, risk-stratified approach that integrates oral glucose tolerance test, self-monitoring of blood glucose, and, whenever possible, continuous glucose monitoring, in addition to relevant hematologic assessments are essential to enhance diagnostic and monitoring accuracy and inform appropriate treatment decisions, especially in primary care and resource-limited settings,” the authors stated.
They argue that OGTT should remain the gold standard for diagnosing diabetes and prediabetes in India, especially in regions with high anaemia or haemoglobinopathy prevalence. HbA1c, they insist, should support diagnosis, not replace glucose-based testing.
For monitoring diabetes, HbA1c should be interpreted alongside fasting and post-meal blood glucose readings. Where available, continuous glucose monitoring can provide a clearer picture of daily glucose fluctuations. Alternative markers such as fructosamine or glycated albumin may be useful when HbA1c results conflict with clinical findings.
Policy distortions can lead to misallocation of resources
At a policy level, the authors caution that national diabetes prevalence estimates based solely on HbA1c may be inflated or distorted, leading to misallocation of health resources.
They call for better assay standardisation, routine screening for anaemia and blood disorders and India-specific diagnostic algorithms.
“In most low- and middle-income regions, isolated elevated HbA1c was more common than isolated elevated FPG [fasting plasma glucose]. In these regions, the use of FPG alone may delay diabetes diagnosis and underestimate diabetes prevalence,” the authors cited from a global study of 117 population-based studies.
The authors conclude with an unequivocal message: “The use of HbA1c as a standalone diagnostic or monitoring tool is often questionable in South Asian populations. Persistently high rates of anaemia, inherited haemoglobin variants, enzymatic red cell disorders, and poorly standardised HbA1c measurement instruments can produce misleading values—leading to underdiagnosis, inappropriate treatment decisions, and delayed initiation of care. As India and neighbouring countries expand their diabetes prevention and management programs, diagnostic algorithms must evolve toward more multiparametric, risk-stratified approaches that integrate clinical, biochemical, and hematologic data.”